Bow legged
Bow legged Bow legs or Genu varum may present from infancy through adulthood and has a wide variety of causes. As it becomes more severe, the patient may exhibit lateral knee thrust and a waddling gait. There may be associated in-toeing and secondary effects on the hip and ankle. The problem may be unilateral, with a functional limb-length discrepancy, or bilateral. The family and medical history may reveal clues to the likelihood of persistence or progression.
Bow legged recognized that up to age 2 years, infants may have physiologic bowing of the lower extremities. The hallmark of this condition is symmetrical and painless bowing, usually associated with in-toeing and often with a propensity for tripping. This problem of Bow legged will resolve spontaneously without treatment with normal growth. All that is required is parental education and periodic follow-up to verify resolution.
The prevalence of this condition is not known, but it is frequent enough to be considered a variation of normal in toddlers. Nevertheless, it is a relatively common cause of parents’ seeking medical attention from their primary care providers, who should be knowledgeable in the triage of these conditions. Radiographs, though optional as a rule, may be needed to differentiate physiologic varus from pathologic conditions that call for treatment.
In normal alignment, the lower-extremity lengths are equal, and the mechanical axis (center of gravity) bisects the knee when the patient is standing erect with the patellae facing forward. This position places relatively balanced forces on the medial and lateral compartments of the knee and on the collateral ligaments, while the patella remains stable and centered in the femoral sulcus.
In children younger than 2 years, physiologic genu varum is common but is self-limiting and innocuous. In older children with pathologic varus, as the knee drifts laterally, the mechanical axis falls in the inner quadrant of the knee; in severe cases, it does not even cross the knee
The recognized etiologies for genu varum include mainly the following:
- Rickets – Hypophosphatemic, nutritional, renal disease
- Skeletal dysplasias – Achondroplasia, pseudoachondroplasia, multiple epiphyseal dysplasia, metaphyseal dysplasia
- Tibia vara (Blount disease) –Infantile, juvenile, adolescent
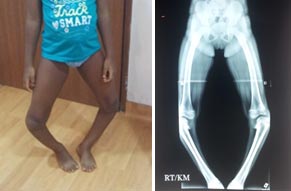

Regardless of the etiology of pathologic genu varum and regardless of the patient’s age, surgical correction of significant and symptomatic malalignment is warranted.
Thorough clinical examination along with appropriate investigations are mandatory to ascertain the cause and the severity of the deformity. In defined metabolic conditions, such as rickets, medical management is paramount for success. There may be other appropriate measures that should be taken according to the problem. Guided growth using 8 – plates is a minimally invasive and modular method of correcting genu varum in the pediatric patient. The key advantage of this intervention is its temporary and reversible nature. At the other end of the treatment spectrum is osteotomy, which involves cutting the femur, the tibia/fibula, or both, depending upon the level or levels of bony deformity.
The outcome of Guided Growth for genu varum is dependent on patient selection and timing. As noted earlier, this technique is contraindicated for physiologic genu varum and will be of no benefit after skeletal maturity has been attained. At least 6 (and preferably 12) months of predicted growth is needed to derive any benefit.
For the remainder of patients, regardless of age or diagnosis, guided growth holds promise for complete correction of the deformity and may reduce or eliminate the need for more invasive osteotomies. For specific endocrinologic conditions, concomitant medical management is required. There are a variety of options for intervention, ranging from attempted bracing to osteotomy. Bracing was popular until the mid-1900s, but enthusiasm for this approach has now largely dissipated as a consequence of problems with brace design and cost, patient noncompliance, and unproven efficacy.
The parents for the success of the procedure, must understand that although the incisions are small and the correction gradual, the onus is on them to return for follow-up appointments at the specified intervals (typically every 3-4 months while the implants are in place).


